Or, if we have Excel, why can’t journalists and bloggers add and subtract, and do sensitivity analysis?
From Dobridge, Hooper, Slok, “Overview of the 2010 Health Reform Bill,” Deutsche Bank Global Economic Perspectives March 31, 2010. [not online]
In our view, there are reasons to question whether the costsavings cited in the bill will actually come to fruition. The biggest cost savings in the bill are projected to come from reducing Medicare fee-for-service (FFS) payment rates ($196 billion in savings), and reducing Medicare Advantage payment rates ($136 billion in savings).8 Many of the fee-for service payment reductions assume that scheduled “market basket” payment increases to hospitals, nursing homes, hospices and others will be reduced each year by the rate of multi-factor productivity growth (which has recently been averaging about 1 percent a year). Over time, however, this will open up a considerable gap between the costs of providing care and the reimbursement rates, which will lead to pressure to increase payments. There is precedence for scheduled payment reductions not actually going into effect. Medicare payments to physicians have been scheduled to be cut each year since 2002, but these cuts have only been implemented once. Since 2003, Congress has taken action each year to prevent the cuts from going into effect and Medicare physician payments were scheduled to be cut by 21 percent starting April 1.
The Centers for Medicare and Medicaid Services, however, have delayed the cuts by about two weeks in order to give Congress time to reconvene and act. With this
precedence, we question whether these new fee-forservice cuts (and the Medicare Advantage cuts) will go into effect entirely as scheduled. The bill also did not
implement a fix for the issue of scheduled Medicare physician payment cuts — CBO estimates that raising payment rates 1.2 percent and restructuring the formula for
payment cuts will cost $208 billion over the next 10 years. Including this fix, the bill would have increased the deficit.An additional cost issue, but a longer-term one, is that the income cut-offs for the bill’s tax increases are not indexed to inflation. The 0.9 percentage point Medicare tax rate increase and the 3.8 percentage point increase on unearned income applies to individuals making $200,000 a year, or couples making $250,000 a year. As those cut-offs are not indexed to inflation, they will cover a growing share of the population over time—similar to the Alternative Minimum Tax. If, like for the AMT, Congress passes “patches” to prevent to tax increases from reaching more families, the bill will not raise as much revenue as scheduled. While this is not an issue for the 10-year budget window, it could be important for the budget after that point.
Point number one is the famous “doc fix”. My observation — this cost would have been incurred even in the absence of PPACA being proposed. So it’s kinda wierd to bring it up as a defect of the bill.
The second, “patch”, issue, which the CBO scoring mentions on page 13-14, is where we will have to wait and see. Perhaps the political scientists can forecast what will happen here.
But let’s start off the debate by assuming not a single dollar’s worth of revenue enhancement is collected, from “Medicare and Other Medicaid and CHIP Provisions Reductions in Annual Updates to Medicare FFS Payment Rates”, as shown in Table 2 in CBO, “H.R. 4872, Reconciliation Act of 2010: Estimate of direct spending and revenue effects for the amendment in the nature of a substitute released on March 18, 2010,” (March 18, 2010). (I don’t think even the most extreme critics think this would happen, but let’s just take the most conservative assumption here.) How would that change our assessment of PPACA relative to the great fiscal disasters of the recent past, EGTRRA, JGTRRA and Iraq (through FY10)? Let’s reprise the graph from this post, appropriately revised.
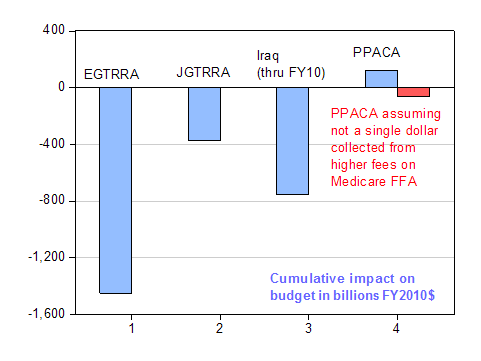
Figure 1: Impact on budget balance, in billions of FY2010$, for EGTRRA; for JGTRRA; cumulative budget authorization for operations in Iraq through FY2010; for Patient Protection and Affordable Care Act, and alternative (red bar) assuming no revenue enhancements from lower Medicare reimbursements; in billions of FY2010$, deflated using CPI. Source: CBO, Budget and Economic Outlook: An Update (August. 2001), Table 1-4; CBO, Budget and Economic Outlook: An Update (August 2003), Table 1-8 (revenue implications only); and CBO, “H.R. 4872, Reconciliation Act of 2010: Estimate of direct spending and revenue effects for the amendment in the nature of a substitute released on March 18, 2010,” (March 18, 2010), Tables 1 and 2; and Iraq costs from A. Belasco, The Cost of Iraq, Afghanistan, and Other
Global War on Terror Operations Since 9/11,
Congressional Research Services (Sep 09), Table 3: budget authorization for DoD, State, and VA Medical; for CPI, historical from FREDII, and forecasts/projections from CBO (January 2010).
Conclusion: Not much impact.
This graph was quite easy to generate. Makes one wonder why those observers so concerned about the possible failure to carry through on revenue-enhancement didn’t generate this graph (or did, but failed to post…). Innumeracy and mendacity are plausible interpetations.
Now, let’s turn to cost savings that CBO excluded. I think this is fair game, because Mr. Samuelson [0] and other critics have listed all the things that CBO did not include because of the parameters of the scoring procedure.
As we discuss in more depth below, rapidly increasing health care costs pose a huge fiscal threat to the US federal budget. There are several key provisions in the bill intended to reduce long-term health care cost growth, with the potential for some significant cost savings in the decades to come. The cost savings will take some time to come on stream, however, and for small test projects designed to lower costs and improve efficiency, there is still considerable uncertainty about whether any cost savings will actually be realized. The state-based health exchanges have the potential to limit cost growth to the extent that they encourage competition among insurers and lead to more transparency about medical pricing. The excise tax on high-cost health insurance plans is another provision that may have an important effect on lowering costs. The tax-advantaged
status of health insurance plans encourages individuals to obtain more generous coverage and consume more health services than they would otherwise, likely driving up medical costs overall. With the excise tax, individuals will face more
of the costs of their high-value insurance, and insurers will have an incentive to reduce premiums. The Council of Economic Advisers estimates that the excise tax could reduce the rate of health care cost growth by 0.5 percentage point a year. The tax is not implemented until 2018, however, which is a long time to wait for these cost savings.9The bill also implements a number of pilot programs geared towards reducing costs. One pilot program would bundle Medicare services for health episodes that include hospitalizations, instead of following the standard fee-forservice
procedure in use today. Bundling care reduces incentives to provide low-value treatments or procedures; recent research has shown that bundling payments for
chronic diseases and elective surgeries could lower medical spending by 5.4 percent through 2019.10 If this program is found to be effective in reducing costs without sacrificing quality of care, it will be rolled out widely. In another
provision, if Medicare cost increases continue to outpace overall inflation, an independent board will be required to submit recommendations for cutting Medicare costs. Unlike most boards tasked with providing recommendations, this Medicare board has a good deal of power to actually have their proposed policies enacted. Their recommendations would go into effect automatically If not acted on by Congress. And if Congress votes against them, but the
President vetoes Congress’s action, the policies will go into effect unless Congress can override the Presidential veto by a two-thirds vote — a high bar.There are a number of other potential cost-saving proposals in the bill as well, including initiatives for value-based payments, which take into account patient outcomes and health status in physician and hospital payments; funding for comparative effectiveness research, which analyzes which health treatments are the most effective; incentives for hospitals to reduce hospital-acquired infections; and the promotion of employer-based wellness initiatives. The CBO projects essentially no budget effects from these measures due to the considerable uncertainty about their cost-containment outcomes. In our view, even if these
programs can substantially reduce costs, we are unlikely to see those reductions for some time. These are small pilot programs, the effectiveness of which will take time to evaluate. If found to be effective, the programs will take
still more time to implement on a large scale. [Emphasis added – MDC]
I think the item emphasized in the quote is one of the measures that Mr. Samuelson thought the plan’s defenders citing was “self-serving and unconvincing”.
The impact of these various measures were deemed as speculative in nature by the CBO. So they weren’t included. Now, here comes the hard part — are the conjectured outcomes of these measures any more speculative in nature than the assertion that none of the revenue enhancing measures will come to pass? Maybe, maybe not. I guess we need some health care economists (here, I do think you need to listen to people with PhD’s) to provide some probability estimates against what the political scientists say is likely to occur (here, I’d like to give more credence to people with PhD’s, but that’s a matter of taste). So, in my view, the plain ol’ CBO scoring is not such a bad place to start, once one recognizes things that were left out on both sides of the ledger.
A parting graphic, for those who are concerned that fiscal apocalpyse will be attributable directly to PPACA+Reconciliation:
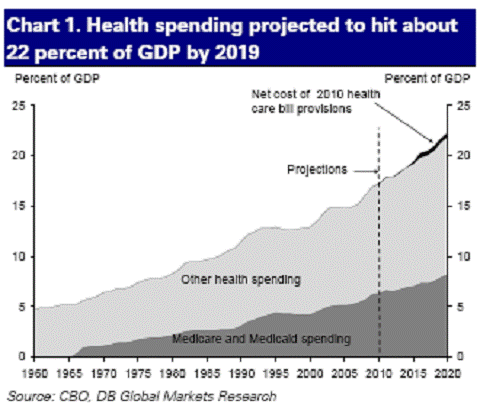
Chart 1 from Dobridge, Hooper and Slok (2010).
I think there are plenty of reasons to worry about fiscal solvency. EGTRRA and Iraq set us on a worrisome path. But PPACA’s contribution is, well, readers can determine for themselves.
See the Committee for a Responsible Federal Budget’s take here.
“Point number one is the famous ‘doc fix’. My observation — this cost would have been incurred even in the absence of PPACA being proposed. So it’s kinda wierd [sic] to bring it up as a defect of the bill.”
It’s not necessarily a “defect” in the bill, but it’s a HUGE factor when considering the costs of the bill.
All involved recognize that the bill with significantly increase the number of services rendered. With current law in place, those services will be discounted by 20% this year and 40% after 7 years – over _today’s_ costs! Unless the bill creates savings that increase proportionally to the costs, when those services are restored to their actual price the “deficit neutral” nature of the reform evaporates.
see here: http://www.broadprinciples.net/2010/03/why-wasnt-doc-fix-counted/
The ‘doc fix’ problem existed before the PPACA was even proposed. It would still exist even if the PPACA never happened. The PPACA never promised to fix that problem so it is hardly fair to blame it on the PPACA. It makes no more sense than blaming the PPACA for not reducing the cost of the Iraq war.
pidgas: See CBPP, Media Matters David Leonhardt. For history and background, see CRS
It’s getting late and I don’t feel like getting my excel out, but the problem I seem to have trouble getting my head around is looking at Chart 1 it shows costs at 18% of GDP (which I thought was the problem) and costs increasing to 22% of GDP over the first 9 years of the plan. (which is worse, right?)
Then how do we say that’s anything like a cost reduction or even revenue neutral?
I never had expectations that PPACA would cost reduce the Iraq War, and they spell it different than TARP, but parts of it smell like EGTRRA, and when spelled out it says “Patient Protection and Affordable Care Act”. Which would lead us to believe it is supposed do something about Affordable Care.
Now of course it would have been nice if we started some of the cost reduction stuff in, say, 2001 instead of beating up on Saddam for being buddies with bin Laden, but we had an idiot for a president back then, and Obama is supposed to be so much better. Why then do I have this feeling we are cooking up another disaster? Granted, what we had was a disaster, but we are running out of Mulligans.
Thank you for some much-needed perspective. On issues relating to fiscal responsibility, it seems that the heat generated is often inversely proportional to the light.
Menzie, this is excellent; you are justifying future spending on the basis of past spending decisions? We splurged in the past and this is a lesser splurge, so all’s well?
Kind of hard to ‘un-spend’ on the other items you mention, so I fail to see the relevance. Ditto all the discussion of “Bush II was so bad” thus the new administration is great…..
Professor Chinn,
I would keep that last graph handy. Republicans always like to hammer some myths (read lies) into the ground like “trickle down” economics and lowering taxes increases the tax base. Professor Chinn I hope you will receive this next sentence like it’s the next best thing to the Gospel of Jesus Christ:
TAKE THAT LAST GRAPH, FIND ANY EXCUSE TO ADD IT TO ANY AND ALL FUTURE POSTS, RUN IT INTO THE GROUND REPEATEDLY UNTIL EVERYONE WHO READS THIS SITE IS NAUSEATED OF IT, AND THEN REPEAT THE PROCESS AD INFINITUM.
Cedric Regula: In Chart 1, the small black area is the net impact of the bill; the other shaded areas are the baselines (under current law). The distinction you are looking for is cost neutral (it isn’t) vs. neutral with respect to the deficit. Under CBO scoring, it is better than revenue neutral. I hope this clears up your confusion.
Dr. D: Thank you for your insight. I guess we should throw away past data. Of course, Mr. Samuelson has indicated the “seeds were sown” for a debt crisis with this measure, and not any of the previous, so I thought there might be some tangential relevance. I regret that you don’t see that relevance.
By the way, just to clarify your worldview, a year ago, you wrote:
I am impelled to ask why you are still reading my posts considering your conclusion made a year ago?
Menzi,
No confusion here. Health care costs sre going from 18% of GDP to 22% of GDP, if whatever you call that thing that passed performs like CBO scored it.
Menzie, does your back ever hurt from carrying the administrations water?
Menzie,
This chart still contains a fundamental error.
The cost-cutting and revenue-generating measures in this bill are not inherent to the expanded spending of the PPACA. They are budgetary moves. The prominent cost cutters that would have been inherent, the public option, reimportation of drugs, and medicare prescription bargaining were tossed out long ago for industry consent.
If the PPACA had simply consisted of the Medicare cuts and increased taxation, as it could have, we would all be on board with you. But when you consider the effect the expansion of entitlements and subsidies has on the budget alone, the chart looks much different.
The PPACA increases government health care spending by over $1 Trillion in the first ten years, but budgetary offsets maintain the fiscal neutrality of the bill as a whole.
Did you happen to account for any offsetting fiscal measures that may have been applied to the other three measures?
And now that we have used up our major health care reform for a generation, soaked up $1T of government revenue, are already paying twice the portion of GDP on health care as any other nation, and are locked into this pattern of spending for a few decades, how can that last passing graphic be anything but a picture of impending doom?
Brad P.: There are a lot of things I would have preferred in this bill, and other bills. I’m just plotting the data, and examining one relevant counterfactual. I’m not sure I understand your criticism that these are budgetary moves. Well, I’m examining a piece of legislation’s impact on … the budget.
joe: Er, do you have a substantive critique?
Ryan has attacked the CBO estimate based on the Republican doc fix which reduces costs in the future, and that Republicans have repeatedly postponed, and then argues he has a better plan for controlling costs because it imposes cost cuts on retirees and insurers in the future.
But we know from Ryan that such future cuts in his Republican plan will always be postponed by Republicans in the future, so Ryan’s plan won’t cut costs.
The Reagan Revolution placed all health care cost control in the hands of the profit motive.
Anyone who has passed intro micro economics knows that profit is what drives up costs to the customers of the firm, because that is the way to maximize profits.
Conservatives argue for basing health care on profit incentives by confusing the debate by purposely confusing price and cost. This is standard profit seeking marketing. Buy two of these $5 widgets for $9 and you will save $1 off the $5 you need to spend; better yet, buy 5 for $23 and you cut the price of the widget you need now to $3 from $5 and protect yourself from future price hikes.
It is no accident that the nations we compete with in global trade have made essential health care services not-for-profit so cost control is possible. It is no accident that the US taxpayer pays more in taxes to fund health care than the Canadian resident pays in total and yet has better quality health care.
Menzie,
I think Brad P is pointing out that cost reduction measures could have been implemented as a stand alone measure. We didn’t need to pass the spending increases.
Since the spending is nearly equal to the costs, this implies we could have chosen to reduce national health care costs by the same $1 trillion that now becomes additional government spending on health care.
If the Progressive Party represented the majority of Americans, they would have solved the debt problem before creating new health care spending. Celebrating the claim that the health care bill is ‘budget neutral’ is like crowing about the fact that the Titanic stopped taking on water once it came to rest on the ocean floor.
Menzie,
The point about the budgetary moves is that you could apply the cost-cutting and revenue-generating measures as offsets to any of the programs.
Supporters of this bill like to lump them with the entitlement expansion, and it is largely arbitrary.
Look at is from this perspective:
You said:
“Point number one is the famous “doc fix”. My observation — this cost would have been incurred even in the absence of PPACA being proposed. So it’s kinda wierd to bring it up as a defect of the bill.”
This is true, expenses that were necessary prior to the PPACA should not be counted against the PPACA.
With that same logic, I look at the extra taxation and cuts in services that are included in the PPACA as necessary prior to PPACA, and so I don’t feel that they should be counted towards the PPACA.
I wouldn’t expect Obama to throw himself under the bus, and he at least managed some decent measures in conjunction with the bill. But he cannot act as if the expansion of entitlements is justified fiscally just because the necessary cuts are coincidental to the optional extra spending.
mulp:
“The Reagan Revolution placed all health care cost control in the hands of the profit motive.”
Even if this were relatively true (it isn’t), the profit motive performs according to plan the vast majority of the time.
You cannot issue the profit motive as a blank pejorative, if it doesn’t work, there must be a reason. In health care, there are a multitude of reasons the market may fail, but you do not list any of them.
There are a lot of “might have beens” and loose ends and unknowns in all these projections. Some might have beens include things that might have been included if the Republicans had been willing to sit down and actually negotiate with the Dems on this bill rather than just saying no. So, an obvious deal that would have lowered costs more would have been a public option for tort reform. The former would lower costs by increasing competition, and the latter would lower costs for well known reasons. Apparently there was never even the remotest discussion of such a deal.
A big unknown is just what will happen to insurance costs once the exchanges are set up. I do not think anybody knows. Of course Menzie is completely correct that the “doc fix” should not be counted as part of the “cost of health care reform.” It was going to happen one way or another anyway.
I might note one other “might have been” that was not remotely on the table, although it would have been an outcome of a single payer plan, which was supported by some in Congress but never got in the door in a serious way, unlike the public option, which nearly went all the way. This would be to ban for-profit health insurance, put them all back to what Blue Cross-Blue Shield was before it got bought out by the for-profit Anthem. Obviously most will view this as some kind of awful socialist heresy, but in fact the only other high income country that does not have a public option and also has for-profit health insurance companies is Switzerland, where there is mandatory coverage of everybody, and those insurance companies are far more heavily regulated than ours will be even after this bill gets fully implemented. The whole idea of for-profit insurance companies is part of why we have even had these scandalous problems such as people being thrown off plans when they make claims or being refused coverage for pre-existing conditions.
For those of you bloviating about coming disasters, please explain how it is that our more privately oriented than any other high income country’s system (with its crappy life expectancy and infant mortality rates) has gotten to cost so much more than any other high income country’s, indeed to the point that the US spends by far a higher percentage of its GDP on its crappily performing health care system? Please explain, Brad P and other whiners.
I will close by noting that there are six different systems out there, and this reform does not fundamentally change ours, really just extends it some and reforms it some. Here they are.
1) pure laissez-faire, not present now in any high income country (and mighty few poorer ones, try Guatemala if you like it)
2) the US mixed system with its non-universal coverage and its for-profit health insurance companies
3) Universal but private systems, Netherlands and Switzerland
4) Universals mixed system with a public option, France (worlds’s best according to the WHO) and Germany
5) single payer universal coverage, but privately employed health care workers, Canada
6) full blown socialized medicine with health care workers employees of the state: UK and former USSR.
Didn’t realize I was whining, but for some reasons why we have artificially high health care costs:
1. Government taking up 50% of all health care spending within a “private” delivery system
2. Separation between consumer and payer (studies have shown that low benefit, low premium, true health “insurance” is very effective in cutting costs and overuse)
3. Subsidies for employer provided health care
4. Lack of caps on health care professional compensation (Doctors in Europe and Japan make a fraction of what American doctors do, and it shows in the skills of American specialists)
5. Competition barriers
6. Americans bear the financial burdens of medical research, with Europeans free riding on that expenditure
There are probably others. Although saying the US health care system is performing crappily isn’t quite fair. In some areas the US is the tops in the world by far.
I still don’t understand.
So, on the cost side, one can’t be disqualified for pre-existing conditions and there is no lifetime spending cap. On the revenue side, you have to pay 1% (rising to 2.5%) of your gross income in taxes if you don’t have healthcare.
So, let’s assume I’m one of those youth who nowadays are prone not to buy healthcare insurance. My income is $40,000, my monthly health insure premium is around $400, about $4,800 on an annual basis. Now, if I drop my insurance, I pay $400 in penalty, save $4,400 per year, and can buy insurnace if I get sick. Or do I have it wrong? What is rational behavior here? Is this what the law actually says?
And then this: “If Medicare cost increases continue to outpace overall inflation, an independent board will be required to submit recommendations for cutting Medicare costs. Unlike most boards tasked with providing recommendations, this Medicare board has a good deal of power to actually have their proposed policies enacted. Their recommendations would go into effect automatically If not acted on by Congress. And if Congress votes against them, but the President vetoes Congress’s action, the policies will go into effect unless Congress can override the Presidential veto by a two-thirds vote — a high bar.”
Is this not functionally a death panel? Are they not going to be the Solomons who decide what gets funded, and what doesn’t? Is that the trick? Does it mean that Medicare will be effectively capped at around 6% of GDP? Does it invalidate the chart above?
Where do savings come from? Is withholding payment imply savings, or rationing?
Is the chart above right? If it is, it’s an unvarnished disaster. Are you going to repudiate it and tell us why the situation really isn’t that bad?
Brad P.,
Your item list at least partially answers it, and there is more as well. I would agree that in certain areas and specialties we are tops. Unfortunately, the problem has been that this tops has not been available to lots, arguably most, people in the US.
Anonymous,
Having the ability cut Medicare spending is equivalent to “death panels”? Really? Please do not tell me that you were one of those tea partiers who is on Medicare who was going around holding signs denouncing “socialized medicine!”
You’re railing against their not doing the math, but the folks you are criticizing are railing (whether they know it or not or are honest about it or not) against the political fact that given the bill as structured, there are many ways in which no bending of the curve will occur and in which there could be significant undoing. I think it is reasonable, given the track record of congress, to be very worried that in a few years there is a cave-in to political pressure which undoes many provisions, including the most important ones for cost containment and the most important ones for coverage in 2014. So, yeah, you’re totally correct that there is either stupidity or dishonesty in the lack of doing the math, but I think a lot of that comes from the fear that the political process can’t handle this thing and will simply find a way to unhinge it when push comes to shove. I’d love to be proven wrong. The first test of many to come is, as you say, in two weeks.
Brad P,
In Europe, Canada and other places, government takes up 100% of health care spending and their per capita costs are much much lower.
Profit motive only works when it is aligned well with the interests of consumers, when there’s sufficient competition and when consumers have access to enough understandable information to make decisions. If you make more money by being more efficient at serving more customers well, than that’s what the profit motive will lead you to do. However, if the chief way to make money is for you to avoid providing service to customers (health insurers) and the only way for consumers to reduce their costs is to avoid paying them until necessary (wait till you get sick) then you’ve got a profit motive misalignment that’s a problem.
Add to that uncompetitive insurance markets and a complete lack of understandable information upon which to base comparisons between competing providers and you get markets that just don’t work.
The bill addresses all three issues — by requiring providers to cover everyone and pay for all needed expenses, they can no longer compete through the avoidance of providing service, but only by obtaining more customers. The Exchanges provide a potentially national market where plans from all over the country will compete and provisions in the law require insurance companies, hospitals and medical providers to disclose all kinds of information about costs and quality of service.
One final point, prior to the 60s and 70s, I believe most medical care in this country was provided by non-profits. So you can maybe understand why people look at the rise of for-profit medicine and blame it for increasing costs.
You make a valid point that the Dems could have just cut the deficit with some of their measures, but that wouldn’t address the larger issue of rising insurance premiums which are a huge burden on businesses. I’ve read somewhere that a significant percentage of small businesses say they’ve had to let people go or not hire because of health insurance costs. And a lot of smart people on this subject think you can’t get costs under control until you have most everyone covered.
tj and Brad P make the salient point. It is misleading to lump the expanded health care with the revenue measures that were needed to address the structural deficit in any event and claim the measure is fiscally responsible. Does this mean that if we were on the brink (if we aren’t already) of fiscal insolvency, it would be responsible to match a tax increase needed to bring us back from that brink with a new extension in entitlements, on grounds that the total measure did not add to the deficit?
Dr. Menzie,
you should read the actual _sources_ the cbpp and mediamatters articles use. They do not support the cbpp/mm conclusions. Read the post I cited.
Pidgas
DS,
I am perfectly willing to admit that the health care delivery system of the US is poor. The strange thing is that health insurance companies have some of the lowest profit margins within the industry, so I can hardly say that these companies are doing much more than passing on the insane costs of health care services.
I will also admit that a single-payer system or public option would be better than what we have or what Obama has signed into law. Health insurance companies should be behaving as proxies on behalf of health care consumers and bringing the costs of health care down.
For whatever reasons (and I would argue reasons that are entrenched by this bill), they are failing at that. A public option or single-payer system would hopefully have supplanted all of the government protections of health care and pharmaceutical providers that health insurance companies couldn’t break through and lead to greater negotiating power on behalf of consumers.
Pidgas: Isn’t this the same guy who believed nothing particularly bad would happen if the stimulus package wasn’t passed? [0]. But even taking his/her point at face value, it seems to me a proper accounting would incorporate those costs into any waiver of the SGR schedule. So, I’ve read the post, and still am wholly unconvinced. Apologies.