Or, “CBO Score — them’s fightin’ words!”.
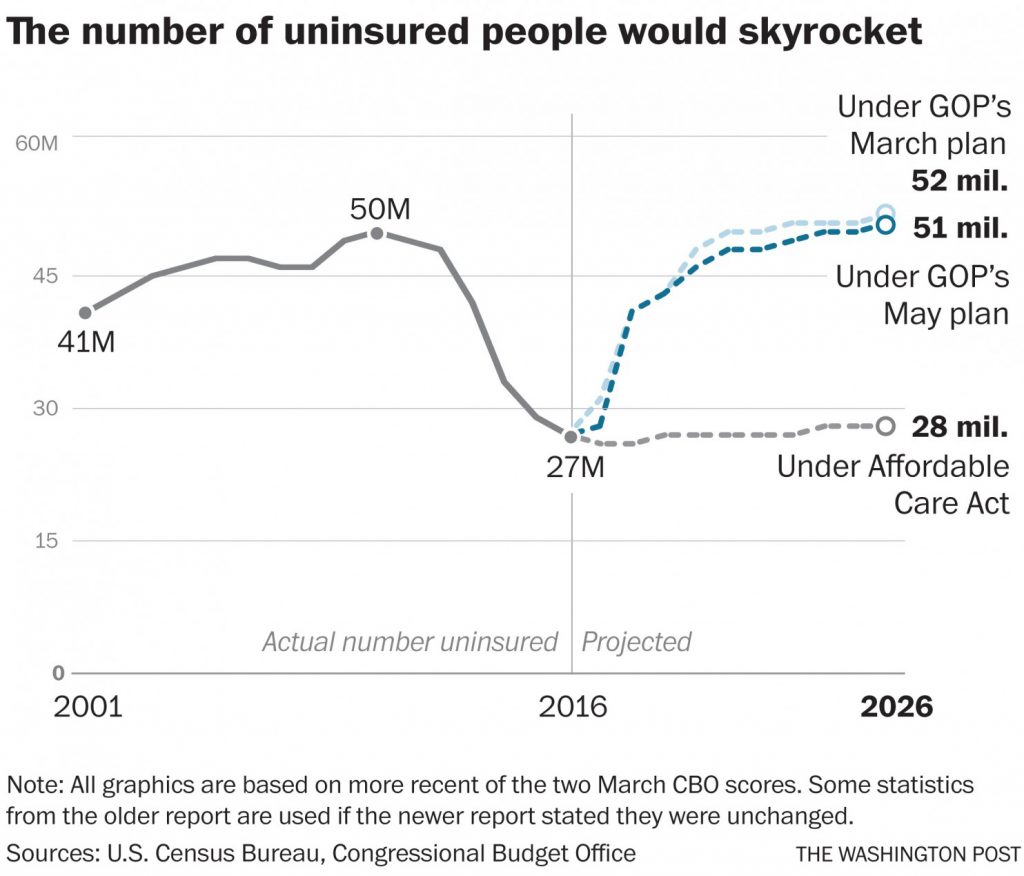
Source: Eilperin, Snell, “Uninsured ranks still to grow by tens of millions under latest House health-care bill, CBO says,” WaPo, May 24, 2017.
From today’s CBO score of the AHCA, bottom line, 14 million more uninsured next year, and 23 million more by 2026.
CBO and JCT broadly define private health insurance coverage as consisting of a comprehensive major medical policy that, at a minimum, covers high-cost medical events and various services, including those provided by physicians and hospitals. The agencies ground their coverage estimates on that widely accepted definition, which encompasses most private health insurance plans currently offered in the group and nongroup markets. The definition excludes policies with limited insurance benefits (known as mini-med plans); “dread disease” policies that cover only specific diseases; supplemental plans that pay for medical expenses that another policy does not cover; fixed-dollar indemnity plans that pay a certain amount per day for illness or hospitalization; and single-service plans, such as dental-only or vision-only policies. In this estimate, people who have only such policies are described as uninsured because they do not have financial protection from major medical risks.
CBO and JCT estimate that, in 2018, 14 million more people would be uninsured under H.R. 1628 than under current law. The increase in the number of uninsured people relative to the number projected under current law would reach 19 million in 2020 and 23 million in 2026. In 2026, an estimated 51 million people under age 65 would be uninsured, compared with 28 million who would lack insurance that year under current law. Under the legislation, a few million of those people would use tax credits to purchase policies that would not cover major medical risks.
Here are a couple of salient graphs, on (1) impact on coverage, and (2) Medicaid coverage.
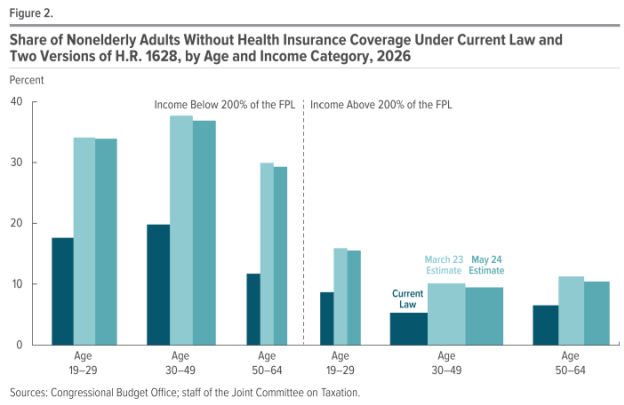
Source: CBO, Cost Estimate: H.R. 1628, American Health Care Act of 2017 (May 24, 2017).
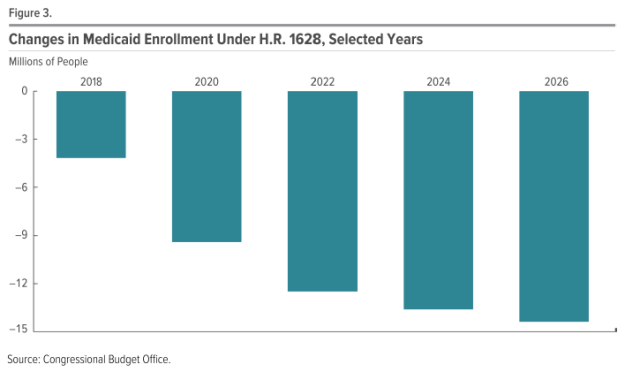
Source: CBO, Cost Estimate: H.R. 1628, American Health Care Act of 2017 (May 24, 2017).
And about pre-existing conditions coverage?
Although premiums would decline, on average, in states that chose to narrow the scope of EHBs, some people enrolled in nongroup insurance would experience substantial increases in what they would spend on health care. People living in states modifying the EHBs who used services or benefits no longer included in the EHBs would experience substantial increases in out-of-pocket spending on health care or would choose to forgo the services. Services or benefits likely to be excluded from the EHBs in some states include maternity care, mental health and substance abuse benefits, rehabilitative and habilitative services, and pediatric dental benefits. In particular, out-of-pocket spending on maternity care and mental health and substance abuse services could increase by thousands of dollars in a given year for the nongroup enrollees who would use those services. Moreover, the ACA’s ban on annual and lifetime limits on covered benefits would no longer apply to health benefits not defined as essential in a state. As a result, for some benefits that might be removed from a state’s definition of EHBs but that might not be excluded from insurance coverage altogether, some enrollees could see large increases in out-of-pocket spending because annual or lifetime limits would be allowed. That could happen, for example, to some people who use expensive prescription drugs. Out-of-pocket payments for people who have relatively high health care spending would increase most in the states that obtained waivers from the requirements for both the EHBs and community rating.
A little more explicitly:
…over time, less healthy individuals (including those with preexisting or newly acquired medical conditions) would be unable to purchase comprehensive coverage with premiums close to those under current law and might not be able to purchase coverage at all.
…
CBO and JCT estimate that a few million people would buy policies that would not cover major medical risks. That estimate is highly uncertain. Although less healthy people might be able to purchase plans that would include a limited number of benefits, those policies would not provide sufficient financial protection to meet CBO’s definition of insurance coverage. The existence of tax credits in the nongroup market would encourage a second market to emerge to sell policies priced to closely match the size of the credits.
Although such plans would provide some benefits, the policies would not provide enough financial protection in the event of a serious and costly illness to be considered insurance.
I see there are pre-emptive attacks on the CBO’s assessment from the usual suspects; see this post for a discussion. For a discussion of CBO’s macroforecasting record (as compared to say the Administration or Blue Chip), see this post.
How many of those not covered have chosen this option because there will no longer be a penalty for going without coverage?
I do not believe it is the role of the federal government to provide insurance for everyone.
do you support the rule that requires emergency rooms to treat everybody, regardless of payment ability?
It definitely needs to be scaled back. If nonprofit hospitals want to provide such care, that’s absolutely great and I support them. But too many people use emergency rooms as health clinics for ailments that are not emergencies.
“If nonprofit hospitals want to provide such care, that’s absolutely great and I support them.”
Only about 20% of hospitals are for profit. the rest are nonprofit and government. so 80% of the hospitals are nonprofit and provide this service as a means to remain nonprofit. what do you want to scale back?
regarding emergencies, you really cannot claim something is not an emergency until after you treat them. a heart attack that is simply heartburn still needs treated. you want to filter patients a priori, but that is very difficult to do.
Is it the role of the federal government to provide very large tax breaks for people who consume health services, including insurance premiums and employer deductibility of insurance contributions? Is it the role of the federal government to sponsor R&D in healthcare research? Or do you mean that the federal government shouldn’t provide insurance for everyone except yourself? I suspect it’s the latter.
Tom: And I’m not sure NRSRO’s should be allowed to exist given agency problems. But I think they might be a second best. Similarly, in the absence of society willing to let poor people die on the streets en masse, is there a way to solve the problem. I agree, if we were willing to let the poor (and middle class) and unlucky be rationed out of health care by price, then all would be solved (at least for the rich and employed w/health insurance). And certainly it would be solved for you — so I am happy for you at least!
For an alternative view, and those interested, read today’s editorial of the Wall Street Journal (printed edition, Thursday, May 25).
Careful when you ask questions about the implications of the new CBO score. At least in Montana, if you ask uncomfortable questions, the Republican Congressional candidate will grab you by the throat with both hands, slam your body to the floor, and then start punching you in the face.
Donald Trump has normalized this sort of fascist behavior and I expect to see more of it.
“History doesn’t repeat itself, but it often does rhyme.”
How How Journalists Covered the Rise of Mussolini and Hitler
http://www.smithsonianmag.com/history/how-journalists-covered-rise-mussolini-hitler-180961407/
Trump Calls the News Media the ‘Enemy of the American People’
https://www.nytimes.com/2017/02/17/business/trump-calls-the-news-media-the-enemy-of-the-people.html?_r=0
Montana GOP Congressional Candidate Cited With Misdemeanor Assault of Reporter
http://www.nbcnews.com/politics/politics-news/montana-congressional-candidate-allegedly-assaults-newspaper-reporter-n764421
‘Body slam every journalist,” Tarrant County (North Texas) tea party group tweets, quicky deletes
https://www.dallasnews.com/news/tarrant-county/2017/05/25/tarrant-county-tea-party-group-deletes-tweet-urging-followers-body-slam-every-journalist
Yeah, yeah, yeah Joseph.
The students at Middlebury College, UC Berkeley, and other schools are all little angels, part of Archangel Gabriel’s army, right?
I have not heard one, repeat: *one*, Democratic politician condemning the violence at those colleges.
i would imagine there would be condemnation if it were a member of congress committing the violence.
an elected member of congress was brought up on charges of assaulting a member of the press. let that sink in. ASSAULT on a member of the press. and yet silence or victim blaming. not surprising.
Small correction: the incident happened the night before the election; he had not been elected.
Second small correction: he was charged with misdemeanor assault, which is different from assault.
Also, the violence at Middlebury and UC Berkeley were done in the name of progressive liberalism, for which many (if not all) Democrats stand. No condemnation ever from them. It’s their base.
not a correction. he was brought up on assault charges. i never said felony assault, but probably is appropriate. why do you support elected officials who commit assault? especially when the violence was politically motivated?
You’re comparing a now-elected member of Congress to angry college students who, when things don’t go their way, resort to violence by committing assault? Maybe not a bad comparison at all. If he were 19.
It’s ridiculous to force consumers to pay for insurance that government made way too expensive, while insurers lose money.
We need two systems – a free market system without the extensive regulations and high standards, and a government system. Health care needs to be free of extensive regulations and high standards that waste an enormous amount of time and money, but makes lawyers rich.
A free market, free of excessive burdens, will result in much lower prices. Therefore, we can afford a government system, like the VA, for those unwilling to buy insurance. Health care should be a normal good, not a luxury good, which consumers cannot afford without lots of money from taxpayers or borrowing.
Peak:
Why exactly do we need two systems?
Do we need two systems in the provision of air conditioners? Do we need two systems in the provision of bread? Do we need two systems in the provision of banking services? Do we need two systems in the provision of jeans? Do we need two systems in the provision of apples?
May I suggest you read this post by Steven Landsburg:
http://www.thebigquestions.com/2017/03/15/information-please/
In this post by Landsburg, you can learn some decent economics, which is in modern times forgotten in so many Econ Departments and so many Econ blogs around.
Manfred, we have a system where people work to buy food and a system of food stamps for those who cannot afford or don’t want to work to buy food.
The big problem is when food costs much more than it should, for everyone.
Government has either raised costs or been unable to reduce costs without reducing quantity and quality. We need a free market solution with a safety net.
It can be a problem, for example, the choice of paying for a private education or receiving a free public education if they’re both equal, since everyone will choose the free public education, unless they have money to squander.
seriously, your statement is pure drivel wrapped in stupidity.
“The big problem is when food costs much more than it should, for everyone.”
this seems to be a statement of an idiot. do you even think before you type? you just type senseless rhetoric with an occasional ideological soundbite thrown in for kicks. are you a bot? it would explain alot.
Baffling, if I had a poor comprehension problem, I’d be hysterical like you. It’s not my problem you’re a intolerant rigid idealogue, who frantically defends failed systems, just because of your misguided socialist beliefs.
once again peak, more drivel. your statements are not even coherent.
“It’s ridiculous to force consumers to pay for insurance that government made way too expensive, while insurers lose money.”
ironic as peaktrader obtains his medical treatment through medicare. you willing to give it up, and get a private policy?
Baffling, you should stop making things up, and support only limited and poor choices.
The American people deserve better choices.
you are a bot!
PT: the odds of your two system idea being seriously considered–much less adopted– are slightly less than the possibility of Disneyland moving from Anaheim to Fresno.
Joseph, he also won the election. Many, many voters are getting and were (the presidential election) tired of the Dem’s/left’s/presses obvious effort to “normalize this sort of lying fascist behavior.” When can we expect to see these absurd exaggerations/lies end?
Yes, he did win the election. This is a sad commentary on the intelligence of Montana voters. His “apology” was wimpy. If he were the tough guy he pretends to be, then he’d “man up” and resign his newly won seat. But he won’t because he’s just another predator politician. Just like Trump.
BTW, this is the third such incident in the last month involving GOP politicians. This one just happened to get more publicity because the audio was so disturbing. There’s a pattern here. A pattern that started long before Trump started campaigning, but Trump was definitely an enabler. Remember his incitements to punch members of the press and offer to pay for their legal fees? Trump might not have been serious (who knows?), but obviously some of his supporters thought he was. Trump should be held accountable for enabling thuggish behavior. But here again, Trump won’t “man up” either.
One Republican misbehaves and it’s front page news all over the liberal media.
If a politician cannot handle rude, disrespectful, and annoying “journalists,” he shouldn’t be running for office.
The CBO track record of projections might leave a bit to be desired:
https://www.forbes.com/sites/theapothecary/2017/01/02/learning-from-cbos-history-of-incorrect-obamacare-projections/#1bfe4fe846a7
I have no idea why you persist in citing articles from Forbes. It’s a p.o.s. rag that’s almost as bad as Faux News. And as usual, Forbes gets plenty of facts wrong, which you would have known if you ever bothered to read serious econ papers. Cancel your subscription to Forbes and buy a subscription to NBER’s working papers.
While CBO was wrong about the internal distribution between the exchanges and Medicaid, CBO was pretty close at the macro level. And most of their forecast error was due to the SCOTUS ruling that allowed states to opt out of Medicaid. The fact is that by 2016 the exchanges had stabilized and were mildly profitable. Next year’s problems are only been because the GOP has done its damnedest to sabotage Obamacare out of spite.
But setting all of that aside, I have no idea why you think the Forbes article strengthens your case. The Forbes article is basically saying that health insurance was in even worse shape than CBO expected. If CBO has a bias towards being too optimistic about the status of health insurance in this country, then isn’t that an argument for thinking the number of uninsured due to the AHCA will be even higher than what CBO projects?
Slugs:
“… and buy a subscription to NBER’s working papers.”
With the economics the you spout day in and day out, I really cannot see that you subscribe to the NBER working papers either. Just sayin’.
2Slug,
Sorry you are personally offended by articles in Forbes. I should have included a trigger warning. But the editors and staff of Forbes didn’t write the article, so I have to presume you are offended by Brian Blase because his political views do not align with yours. However, dismissive remarks need to have some credibility. Would you care to elaborate?
Brian Blase bio:
“I am a senior research fellow with the Spending and Budget Initiative at the Mercatus Center at George Mason University. I focus on health policy, particularly the implementation of the Affordable Care Act and the nation’s entitlement programs. I joined Mercatus in August 2015 after nearly four-and-a-half years working on Capitol Hill, serving first as a senior professional staff member for the House Committee on Oversight and Government Reform and then as the health policy analyst for the Senate Republican Policy Committee. I advised Senator John Barrasso in his role leading the Senate Working Group tasked with developing a legislative response if the Supreme Court ruled for the plaintiffs in the King v. Burwell case, striking down exchange subsidies in two-thirds of the country. Prior to working for Congress, I was a health policy analyst for The Heritage Foundation. I have a PhD in Economics from George Mason University, completing a dissertation on Medicaid financing.”
2Slug bio:
For a different view on things, read Bob Kerrey’s Letter to the Editor in today’s Wall Street Journal (Friday, May 26). And keep in mind, Bob Kerrey is a Democrat.
In his short letter, there is a statement like this:
“In the past 100 years every federal intervention in health care has made things better for the beneficiaries, but worse for those paying the bills.”
I never would have expected that a modern day Democrat would make a statement like this. Maybe there is a God after all.